The postpartum period, or the year following the birth of a child, represents a significant opportunity for reaching women with effective family planning, reducing the likelihood of unintended pregnancy and increasing the likelihood of healthy birth spacing. During pregnancy and childbirth, as well as during the year following childbirth, women are more likely to engage with the healthcare system during antenatal care, delivery, postnatal care, and first year infant immunizations. Each of these encounters is an opportunity for health care workers to integrate family planning into their existing counseling and services to better meet the needs of postpartum women. For example, the WHO recommends that all postpartum women receive a post-natal visit at 6 weeks. This visit represents an opportunity to assess women's return to fertility, counsel them on their contraceptive options, and provide a contraceptive method. At this time, postpartum women are eligible for all modern methods of contraception (except combined pills for women who are breastfeeding).1
Analysis of DHS data from 27 countries found that across nearly all of the sampled countries, as many as 9 in 10 postpartum women wanted to delay their next pregnancy for at least 2 years.2 This desire is consistent with WHO recommendations of an interval of at least 24 months between delivery and attempting the next pregnancy to reduce negative health outcomes for women and their infants. However, this same analysis found that among postpartum women there is substantial unmet need for family planning, with an average of 65% of women across the countries analyzed citing a desire to delay or avoid another pregnancy but not using contraception.3 As return to fertility and sexual activity vary widely by individual and country context, providing all postpartum women with access to family planning in the weeks and months immediately following delivery is essential to ensuring they are able to avoid unintended pregnancy and achieve their fertility desires.
Track20 analyzed DHS data from 36 FP2020 countries to assess the timing of uptake of family planning over the first year following delivery. The analysis uses data from 36 DHS surveys conducted from 2002 to 2016. Building on the methodology used by Winfrey and Borda (using DHS Calendar data), we looked at modern contraceptive use by months since delivery, in the year following delivery and using the DHS definition of modern contraceptive methods. This analysis aims to look at levels of postpartum contraceptive use among postpartum women over the first year postpartum; see our 'Opportunities for Growth' section of the website for analysis the looks at the potential of PPFP interventions to increase national level contraceptive use by looking at postpartum non-users as a proportion of all women in each country.
Here we present some overall results. Use the tool below to explore country level results by region. Among women at one month postpartum, the unweighted average modern contraceptive prevalence was 8%, ranging from 0% in Burkina Faso to 44% in Zimbabwe. By the 12th month postpartum that unweighted average increases to 30%, ranging from 6% in Benin to 72% in Indonesia.
On average, the largest increase in prevalence occurs between 1 and 2 months postpartum (an average of 8% pts or an increase of 97%). The most rapid growth in prevalence is seen in Egypt, where postpartum contraceptive use increases from 5% to 62% between 1 and 2 months postpartum. In half of the sampled countries, the largest increase in utilization of postpartum family planning occurred between 1 and 2 months postpartum.
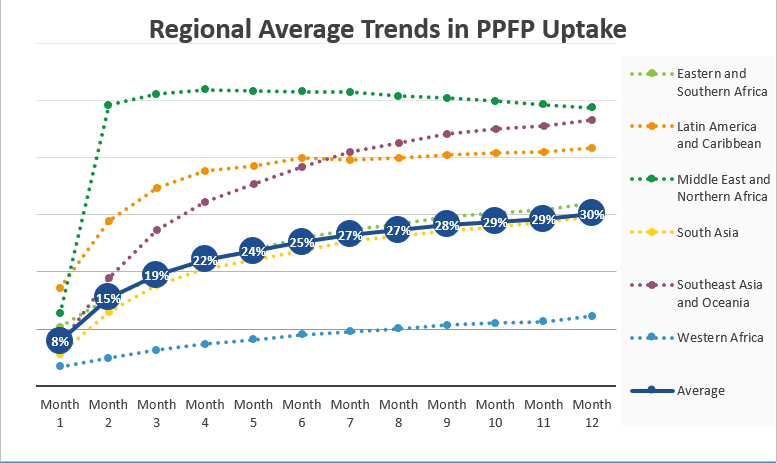
The increase in modern contraceptive prevalence between 1 and 2 months seen in many of the analyzed countries may indicate contexts where the WHO recommended 6-week visit is being utilized to counsel on and deliver postpartum contraceptives.
Use the dropdown list below to review these trends in postpartum family planning uptake by region:
[1] Report of a WHO Technical Consultation on Birth Spacing
[2] Contraceptive Use, Intention to Use and Unmet Need During the Extended Postpartum Period
[2] Programming strategies for Postpartum Family Planning